Cedar fever symptoms can strike suddenly and severely, leaving you sneezing, congested, and exhausted through the heart of winter. If you’ve ever wondered why your eyes itch relentlessly and your nose won’t stop running in January, you’re likely experiencing the hallmark cedar fever symptoms that affect millions each year.
You wake up on a crisp January morning, feeling unusually groggy. As you sit up, your nose begins to run; a fit of sneezing follows. Your eyes sting and water uncontrollably, and a dull headache settles behind your brow. You might think it’s a lingering cold or “just the flu,” but if these symptoms persist—especially without a true fever—you’re probably battling cedar fever symptoms.
Despite the name, cedar fever isn’t a fever. It’s a severe allergic reaction to pollen from mountain cedar (Ashe juniper) trees. These trees release massive amounts of pollen in late fall and peak in January, triggering the characteristic cedar fever symptoms. Understanding cedar fever symptoms early allows you to seek proper treatment rather than enduring ineffective cold remedies.
For reliable medical information on cedar fever, see Cleveland Clinic’s overview of cedar fever symptoms and treatment.

This comprehensive guide dives into everything you need to know about cedar fever symptoms:
- Why cedar pollen causes such intense reactions
- How cedar fever symptoms differ from colds and flu
- Real-world case studies and examples
- A detailed symptom occurrence table and seasonal severity graph
- Effective over-the-counter, prescription, and lifestyle treatments
- Q&A addressing your most pressing cedar fever questions
By recognizing cedar fever symptoms and taking proactive steps, you can reclaim your winter months—free from relentless sneezing, itchy eyes, and unshakable fatigue. Read on to learn how to identify, manage, and overcome cedar fever symptoms this season.
Table of Contents
The Telltale Cedar Fever Symptoms to Watch For
The allergic reaction to mountain cedar pollen can feel like a full-body assault. While it shares some characteristics with a common cold, the symptoms are often more severe and persistent. Here are the most common cedar fever symptoms you might experience:
- Intense and Persistent Sneezing: Not just a sneeze here or there, but uncontrollable fits of sneezing that can be disruptive.
- Runny Nose and Nasal Congestion: You’ll likely have a constantly running nose with thin, clear mucus. This is a key differentiator from many bacterial infections, which often produce colored mucus. This can be accompanied by a stuffy, congested feeling.
- Itchy, Watery, and Red Eyes: This is one of the most significant signs of cedar fever. The itchiness can be severe and is a classic symptom of an allergic reaction rather than a cold.
- Overwhelming Fatigue: A profound sense of tiredness and malaise that feels disproportionate to the other symptoms. This exhaustion is a result of your immune system working overtime.
- Sore Throat and Nagging Cough: Often caused by post-nasal drip from your runny nose irritating your throat, rather than a primary infection.
- Sinus Pressure and Headaches: The inflammation in your nasal passages can lead to painful pressure behind your eyes, cheeks, and forehead, often resulting in a persistent headache.
- Plugged or Popping Ears: The sensation of your ears being full or needing to “pop” is common due to pressure changes in your sinuses.
- Partial Loss of Smell: The severe congestion can temporarily block your olfactory receptors, making it difficult to smell properly.
- A “Feverish” Feeling (Without a High Fever): While cedar fever doesn’t cause a true fever, the inflammatory response it triggers can slightly raise your body temperature, making you feel warm and unwell. A high-grade fever, however, typically points to a viral or bacterial infection.
How Common Are These Symptoms?
To give you a better idea of what most people experience, here is a breakdown of the most frequently reported cedar fever symptoms.
cedar_fever_symptoms.csv
Generated File
| Symptom | Occurrence Rate (%) |
|---|---|
| Runny Nose | 85 |
| Nasal Congestion | 80 |
| Itchy Eyes | 75 |
| Sneezing | 70 |
| Cough | 65 |
| Sinus Pressure | 55 |
| Headache | 50 |
| Fatigue | 40 |
When Cedar Fever Strikes: Understanding the Season
One of the biggest reasons cedar fever is so confusing is its timing. While we associate spring with blooming flowers and allergies, Ashe juniper trees are unique. They pollinate in the dead of winter.
The cedar fever season typically begins in late November, gains momentum in December, and hits its absolute peak in January. Symptoms can often linger through February and even into early March before subsiding.
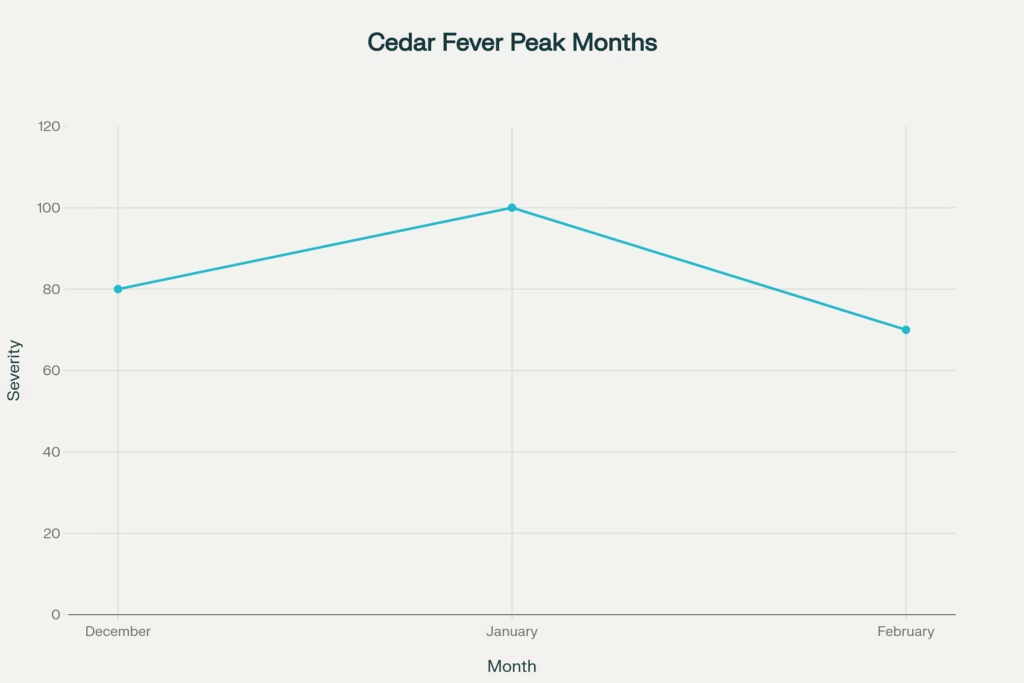
Peak months for cedar fever symptoms severity
This peak often coincides with a specific weather pattern. Juniper trees tend to release their pollen all at once right after a cold front passes through, when the air is dry and the wind picks up. This sends clouds of pollen—sometimes visible, looking like smoke coming off the trees—drifting for hundreds of miles.
This phenomenon is most intense in regions with a high concentration of these trees, including Central Texas, Oklahoma, Missouri, Arkansas, and parts of Arizona and New Mexico.
Cedar Fever vs. Cold vs. Flu: Spotting the Difference
It’s easy to get confused when you’re feeling miserable. Let’s break down the key differences between these common winter ailments.
A Real-Life Example: Sarah’s Story

To illustrate the difference, consider this case study:
Sarah, a 34-year-old graphic designer in Austin, Texas, started feeling sick in early January. It began with a scratchy throat and a runny nose. “I just thought I caught the bug my coworkers had,” she said. She took over-the-counter cold medicine, but her symptoms only worsened. A week later, she was exhausted, sneezing constantly, and her eyes were so itchy and red that she could barely look at her computer screen.
The biggest clue for Sarah was the lack of other “sick” symptoms. She didn’t have a fever or body aches, which she usually got with the flu. Her mucus remained stubbornly clear. She also noticed her symptoms were significantly worse after her morning walks. After a visit to an allergist, she was diagnosed with a severe allergy to mountain cedar pollen. Her doctor prescribed a nasal steroid and antihistamine eye drops, which provided relief within a couple of days.
Sarah’s experience highlights the classic pattern of cedar fever symptoms: the intense itchiness, the clear nasal discharge, and the link to outdoor exposure are all hallmarks of this powerful winter allergy.
Looking for more health tips? Our blog on Vital Health Productos – Your Ultimate Guide to Wellness and Longevity will be helpful
How to Manage and Treat Cedar Fever Symptoms
You don’t have to suffer through winter. Once you know what you’re dealing with, you can take effective steps to find relief. Treatment strategies fall into three main categories.
1. Over-the-Counter (OTC) Remedies
For many people, a combination of non-prescription options can effectively manage symptoms:
- Antihistamines: Medications like Zyrtec, Claritin, or Allegra can help control sneezing, itching, and a runny nose. Medicated eye drops can specifically target itchy eyes.
- Nasal Steroid Sprays: Sprays like Flonase or Nasacort work by reducing inflammation in the nasal passages. They are highly effective but may take a few days to reach their full effect. They are often considered a first-line defense.
- Saline Nasal Rinses: Using a neti pot or a saline squeeze bottle to gently flush your nasal passages can wash out pollen and mucus, providing immediate relief from congestion.
- Decongestants: For severe stuffiness, short-term use of a decongestant like Sudafed can help, but they shouldn’t be used for more than a few days at a time.
2. Prescription and Long-Term Treatments

If OTC solutions aren’t enough, it’s time to see a doctor or an allergist. They may recommend:
- Prescription-Strength Medications: Your doctor can prescribe more powerful versions of nasal sprays, antihistamines, or anti-inflammatory drugs.
- Immunotherapy (Allergy Shots or Drops): For those with severe, recurring cedar fever, immunotherapy can be a game-changer. This long-term treatment involves exposing your body to tiny, controlled amounts of the allergen, which helps your immune system become less reactive over time.
3. Lifestyle Adjustments and Prevention
Prevention is your best weapon against cedar fever. Minimizing your exposure to pollen can make a huge difference.
- Track Pollen Counts: Pay attention to your local weather forecast, which often includes daily pollen levels. On high-count days, try to stay indoors as much as possible.
- Keep Your Indoor Air Clean: Keep windows and doors closed. Use high-efficiency HEPA filters in your home’s air conditioning system and vacuum cleaner to trap pollen particles.
- Create a “Pollen-Free” Zone: When you come home after being outside, take off your shoes at the door, change your clothes, and take a shower to wash pollen off your skin and hair.
- Protect Yourself Outdoors: If you must be outside on high-pollen days, wear a hat, sunglasses, and a mask to help block pollen from getting into your eyes, nose, and lungs.
Q&A: Your Top Questions About Cedar Fever Symptoms
Here are answers to some of the most common questions people have about cedar fever.
Q1: Can cedar fever actually cause a fever?
A: It’s very rare for cedar fever to cause a true, high-grade fever. However, the intense inflammation from the allergic reaction can sometimes cause a slight rise in body temperature (below 100°F), making you feel “feverish” or unwell. A temperature over 100°F almost always indicates an infection like the flu or a cold.
Q2: Why do I feel so incredibly tired with cedar fever?
A: The extreme fatigue is one of the most debilitating cedar fever symptoms. Your immune system mistakenly identifies the cedar pollen as a dangerous invader and launches a massive inflammatory response to fight it. This internal battle consumes a tremendous amount of energy, leaving you feeling completely drained.
Q3: How long do cedar fever symptoms last?
A: Unlike a cold that typically resolves in 7-10 days, cedar fever symptoms will persist as long as the pollen is in the air. This can mean suffering for several weeks or even the entire winter season, from December through February, if you don’t treat the allergy.
Q4: I don’t live in Texas. Can I still get cedar fever?
A: Yes. While the highest concentrations of mountain cedar trees are in the south-central U.S., their pollen is incredibly light and can be carried by wind for hundreds of miles. People in neighboring states and beyond can experience symptoms when a strong weather front carries the pollen into their area.
Q5: Will cutting down the cedar trees in my yard help my symptoms?
A: Unfortunately, this is unlikely to make a difference. The problem isn’t just a few local trees; it’s the massive volume of airborne pollen traveling from vast forests. Your exposure comes from the air around you, not just your immediate yard.
Looking for more health tips? Our blog on Unlock the Life-Changing ROAM Diet: Your Ultimate Guide to Effortless Healthy Living will be helpful.”
Take Back Your Winter
Living with severe cedar fever symptoms can feel like putting your life on hold every winter. But by learning to recognize the signs, understanding what makes this allergy unique, and taking proactive steps to manage your exposure and treat your symptoms, you can significantly reduce its impact.
If you suspect you have cedar fever, don’t just “tough it out.” Talk to your doctor or an allergist. The right diagnosis and treatment plan can transform your winter from a season of misery into one of health and well-being.
Medical Disclaimer
This article is for informational purposes only and is not intended as medical advice. Cedar fever symptoms can overlap with other conditions, and proper diagnosis requires professional evaluation. Always consult with a qualified healthcare provider or allergist before starting any treatment regimen. If you experience severe symptoms, difficulty breathing, or high fever, seek immediate medical attention. Individual responses to treatments may vary.




